Individualized Treatment Planning and Individual Therapy- Part 2
The initial assessment allows us to determine the needs of each patient. This includes determining the need for hospitalization and whether the program is a therapeutic fit. Some patients may need more structure, such as a residential experience, or less, such as an evening outpatient program. We follow the ASAM patient placement criteria but recognize the special needs of some of our patients: for example, our healthcare professionals, who may need to be out of the workplace for a period of time for their own and their patients’ protection. We also evaluate (sometimes on an ongoing basis) whether the independent living program (ILP) is viable, as some patients may need to commute. This can be the case if there are childcare issues or if patients have certain necessary supports in the home. In any case, all patients, whether commuting to the program or living in the ILP, participate in the social support functions that happen around the ILP after hours and on weekends, as outlined later.
Individualized Treatment Planning and Individual Therapy
In the program, each patient is assigned a primary counselor with whom they work both individually and in small groups. This way the counselor knows the patient both in a group setting as well as individually. By virtue of this knowledge, along with additional information from history, family, and psychological testing, including the TCI self-reports, the individual therapist can create a treatment plan that relates to the unique individual needs of each patient.
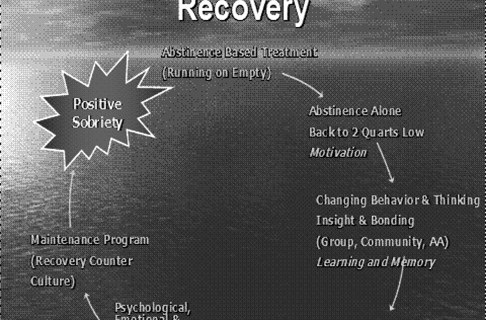
As each of the three elements (the psychological, environmental, and biological) contributes in varying degrees to addiction and all illnesses, in order for any treatment to be fully effective, each element needs to be addressed. The psychological element is addressed in the small group experience, the larger therapeutic community, AA, and didactic parts of the program, and individually with the primary counselor.
A recent review of the literature about the quality of clinicians and substance use disorder treatment outcomes highlights the importance of the individual impact of clinicians on their patients. Evidence suggests that clinicians are a key factor in influencing treatment outcome and retention. Use of written treatment protocols has been noted to increase overall patient outcomes and to reduce variance by clinicians. We have been fortunate to have highly skilled, compassionate, and committed primary counselors in our program.
Incorporating individual therapy into a treatment regimen is an effective means to address underlying psychological issues for some of our patients. Our preference is that, at least initially, the patient connects with the program in the first 2 to 4 weeks of day hospital before engaging in individual work. As the patient steps down to an intensive day outpatient setting, he or she will have more time to see an individual therapist for special needs (e.g., trauma work). Individual work does happen with the primary counselor, but sometimes more is needed. Most patients are recommended to individual therapy after they complete treatment. We have been impressed with the benefits of cognitive behavioral therapy (CBT). CBT addresses the negative self-talk and negative core beliefs that have been present in so many of our patients. CBT has been an effective treatment for many conditions, including depression, anxiety disorders, and addiction (when used as an adjunct to a treatment program regimen). In fact, many patients need to address their negative self-talk before they can effectively use meditation as a way to observe these thoughts.